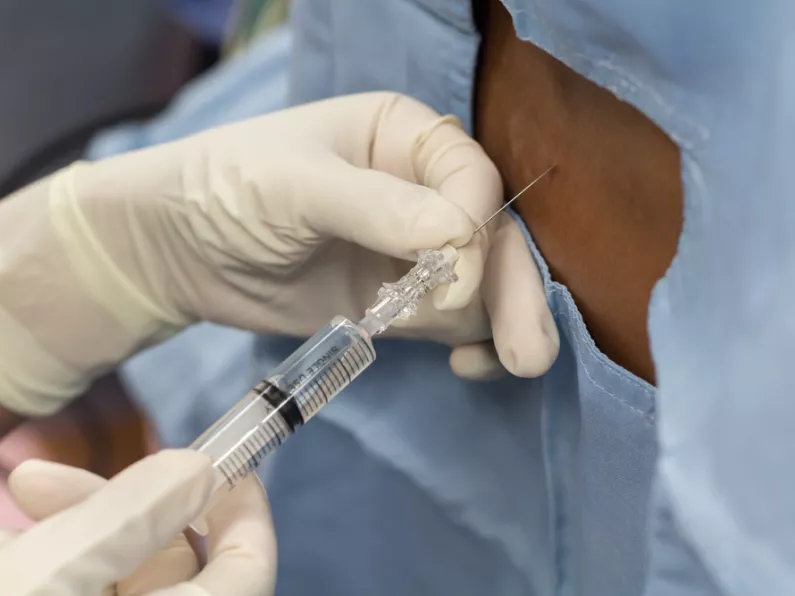
If you're pregnant, TTC (trying to conceive) or already a mom, chances are you'll have had - or at least heard of - spinal blocks and epidurals.
If you haven't, don't worry - you've come to the right place.
In short, epidurals are most commonly used for women anticipating a vaginal birth while spinal blocks are typically used for scheduled or routine c-sections.
But there's more to it than that. So let's dive straight in.
Spinal block vs epidural: what you need to know
What is a spinal block?
Spinal blocks are most commonly used to numb moms prior to a c-section.
It's a procedure that involves an anaesthetist injecting anesthetic below the spinal column, directly into the spinal fluid.
This provides pain relief for up to 2 hours.
What is an epidural?
An epidural is a type of regional anesthesia that blocks pain in a particular part of the body.
The goal during birth is to provide pain relief, rather than completely eliminating all feeling and sensation.
With an effective epidural, you should not feel sharp contraction pain, but you might still feel pelvic and rectal pressure as your baby gets lower into your pelvis.
It typically takes about 20 minutes to feel the full effects of the epidural once it’s placed.
And in that time you'll notice your contractions beginning to feel shorter and less painful.
When is a spinal block used vs an epidural?
When it comes to labour and birth, spinal blocks are most often used for scheduled and routine c-sections.
But placing a spinal block takes a bit of time, so if you or your baby’s condition is unstable and your provider is requesting an emergency c-section, there likely wouldn’t be enough time for a spinal block.
An epidural is used if you're in labour and anticipating a vaginal delivery.
But remember; you may end up needing a c-section if your Obstetrician deems it necessary.
Some examples would be:
- failed induction
- failure to progress
- fetal intolerance of labor.
Similarities and differences
There are a few similarities between epidurals and spinal blocks, including:
- Both provide pain relief for childbirth
- Both work by blocking the transmission of pain signals
- You will be in the same position for the placement of both
- Both are placed by a member of the anesthesia team.
The main differences between epidurals and spinal blocks are:
- Onset: epidurals take about 20 minutes to provide relief whereas with a spinal block, it’s almost immediate
- Catheter: with an epidural, a catheter remains in your back to deliver continuous medication until delivery. With a spinal block, the needle is immediately removed once the medication is administered – nothing remains in your back
- Mode of birth delivery: epidurals are most commonly used for anticipated vaginal births, while spinal blocks are used for c-sections.
Advantages of using an epidural vs a spinal block?
The main advantage of an epidural is the it offers pain relief for a longer period of time.
Once the catheter is threaded into your epidural space, the anaesthetist will administer a test dose of medication to confirm.
If all is well, they will leave the small catheter in your back and tape it down so that it stays in place until you deliver your baby.
The other end of the epidural catheter is connected to a pump that administers pain medication throughout delivery.
With a spinal block, a needle is used to administer the numbing medication and then it's removed immediately.
This is because a c-section typically takes less than 2 hours so the medication doesn't need to work for any longer.
One disadvantage associated with an epidural is that the catheter remains in your back and can be uncomfortable.
Another is that it takes about 20 minutes to start working (a long time when you're in pain!)
Common side effects of both are low blood pressure, nausea and vomiting.